Arizona sober living crisis: 140 indicted in billion-dollar Medicaid scheme
140 indicted in massive sober living house scheme
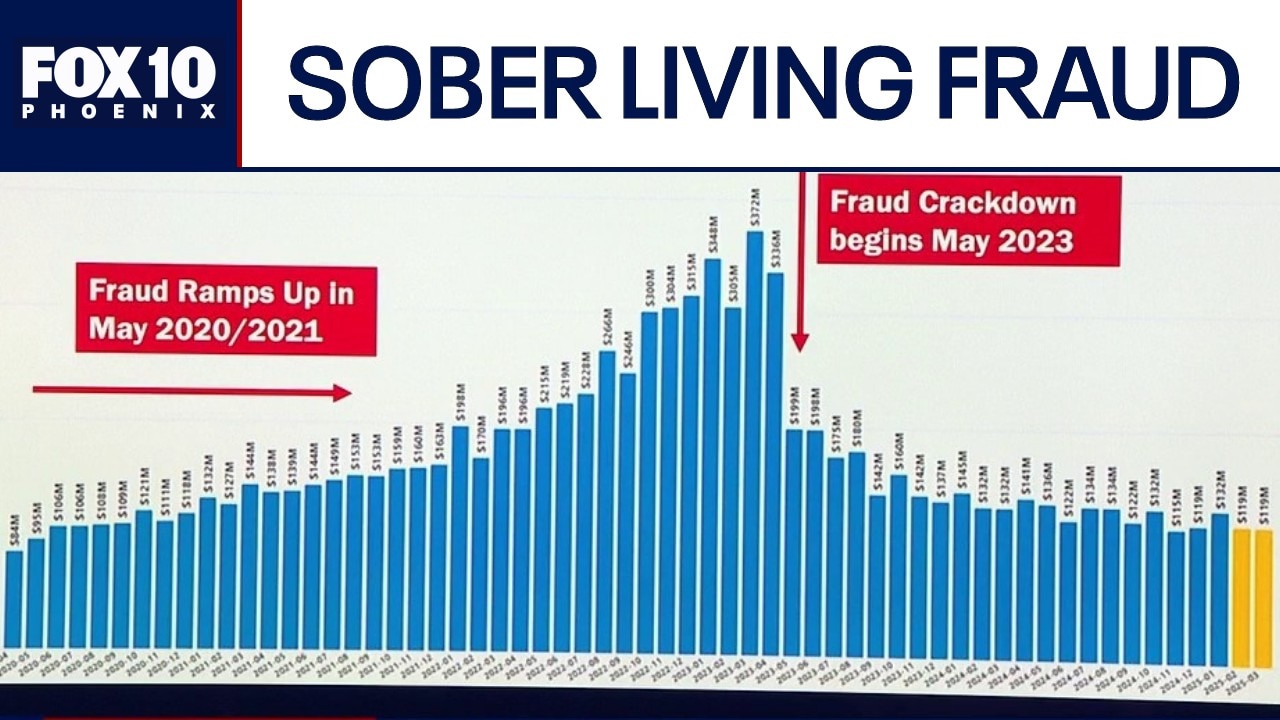
Arizona sees a 92% decline in fraudulent health plan billing following proactive state crackdowns.
PHOENIX - New developments have emerged in the massive sober living crisis in Arizona, a scheme that preyed on vulnerable people and stole billions of taxpayer dollars.
On May 14, Arizona Attorney General Kris Mayes provided an update on her efforts in prosecuting the criminals behind the fraud.
The backstory:
It is a scheme that FOX 10 investigators have covered for more than four years. Vulnerable people battling addiction were preyed upon by bad actors who promised rehabilitation services but rarely provided any. Many of the victims were Native Americans who were kidnapped from reservations and housed in unlicensed and unregulated sober living homes across Arizona. In some cases, victims died when the systems that were supposed to protect them failed.
What they're saying:
The attorney general announced significant gains in the fight to help right the wrongs, including 140 indictments related to these schemes and millions of dollars recovered. Mayes said nothing can fully make up for what happened to these victims, but she is doing everything in her power to make sure it does not happen again. Top Arizona officials are announcing a proactive push to combat healthcare fraud.
"Arizona is a national leader in combating Medicaid fraud because we made it a priority," Mayes said.
Mayes said behavioral health code billing on the American Indian Health Plan has seen a 92 percent decline since her office took action in 2023. More than 140 people and entities related to the fraud have been indicted, including nurse practitioner Rita Anagho, who was sentenced to 3.5 years in prison in the state’s case against her.

Rita Anagho
"Anagho’s scheme deprived legitimate Medicaid beneficiaries of critical resources and, by exploiting an already vulnerable population, helped fuel Arizona's large-scale behavioral health crisis," Mayes said.
Governor Katie Hobbs announced Thursday she’s launching a new AI tool through Arizona’s Health Care Cost Containment System this July to detect and fight fraud. The Medicaid claims prepayment review system uses AI to rank claims for fraud, waste, and abuse before a payment is made. This all comes after the state has spent the last few years recovering from a massive billion-dollar fraud scheme, with vulnerable people on Arizona’s American Indian Health Plan paying the price.
"This fraud was allowed to metastasize largely because the people in charge prior to 2023 were asleep at the wheel, and we have the stats to prove it," Mayes said. "I know that no number of indictments or convictions or amount paid back in restitution can undo the pain and heartbreak and suffering caused by this scandal. But please know that we have heard your stories, and we have seen the damage that has been done."
On May 13, Vice President JD Vance announced that states could lose federal funding for failing to aggressively pursue Medicaid fraud. Mayes claims Arizona is at the forefront of that pursuit.
The Source: Announcements from Arizona Attorney General Kris Mayes, Arizona Governor Katie Hobbs, and Vice President JD Vance; along with previous FOX 10 reporting.

